Endometriosis Naturopathic Support
Endometriosis can affect the whole body. My approach looks beyond the endometriosis lesions alone and explores what may be driving your symptoms underneath, so your plan feels targeted, evidence-aware, realistic, and effective.
What Is Endometriosis?
Endometriosis involves tissue that behaves like the lining of the uterus growing outside the uterus, most commonly within the pelvis. But it’s not only about where the tissue is. It’s also about how your immune system, hormones, and nervous system are responding over time.
This is why two women can have similar surgical findings but very different lived experiences.
What Can Drive Endometriosis Symptoms?
Endometriosis rarely has one simple cause. It’s usually a mix of factors that interact over time. Some may apply strongly to you, while others may not apply at all.
Hormones, including stress hormones
Endometriosis is hormone-sensitive, but it’s not simply a case of “too much oestrogen.” What often matters is how hormones are regulated, processed, and buffered within the body.
Chronic stress affects more than mood. Stress signals begin in the brain and influence adrenal hormones such as cortisol and DHEA. These stress hormones interact closely with cycle hormones, immune signalling, and inflammation.
When stress is ongoing, this regulatory system can become dysregulated. Over time, this may contribute to increased inflammation, heightened pain sensitivity, fatigue, sleep disruption, and a greater tendency toward symptom flares, even when standard hormone tests appear within reference ranges.
For this reason, endometriosis support cannot focus on hormones or inflammation in isolation. Nervous system regulation, sleep, and recovery capacity are often relevant parts of the picture.
Inflammation is the smoke, not the fire
Inflammation is a major feature of endometriosis, but it helps to think of it as the body’s alarm signal — the smoke, not the fire.
The key question is what is keeping inflammation switched on. This can include hormone signalling, gut factors, immune activation, histamine, infections, nervous system overload, or environmental exposures. If we only try to suppress inflammation without addressing its drivers, symptoms often return.
Immune function, gut health, histamine, and iron
Endometriosis is increasingly understood to involve immune dysregulation. Some researchers describe it as having autoimmune-like features, meaning immune responses may become misdirected, even though endometriosis is not classified as an autoimmune disease.
Much of immune signalling is coordinated through the gut. When the gut microbiome is disrupted or the gut lining is inflamed or overly permeable, immune responses can become more reactive and harder to settle. This helps explain why digestive symptoms and food reactions are so common in endometriosis.
Histamine can also play a role. Histamine is a natural immune messenger, but when levels are elevated or clearance is impaired, it can worsen pelvic pain, heavy or painful periods, bloating, fatigue, headaches, sleep disruption, teeth grinding, and anxiety-type symptoms. Histamine and oestrogen can amplify one another, creating flare patterns in some women. Environmental triggers such as mould exposure may further contribute in histamine-sensitive individuals.
Iron regulation can also be complex. Chronic inflammation can alter iron absorption, transport, and utilisation, sometimes leading to functional iron deficiency even when intake appears adequate. At the same time, repeated bleeding and local iron accumulation within endometriotic tissue can contribute to oxidative stress and inflammation. This is why iron support needs to be individualised and assessed carefully, rather than based on ferritin alone.
What the microbiome is and why it matters
The microbiome refers to communities of bacteria and other microbes living in and on the body. These microbes influence immune balance, inflammation, hormone metabolism, and pain signalling.
In endometriosis, three microbiomes are commonly considered:
- the gut microbiome
- the vaginal microbiome
- the uterine or endometrial microbiome
Disruption in these ecosystems may contribute to pelvic inflammation, digestive flares, immune activation, and fertility challenges.
Gut factors that can flare endometriosis symptoms
The gut is one of the body’s largest regulators of immune and inflammatory activity. When the gut is irritated, inflammatory compounds and immune triggers can have system-wide effects.
One example is LPS, a bacterial by-product that strongly stimulates immune responses. This helps explain why IBS-type symptoms, bloating, constipation, diarrhoea, and food reactions often travel alongside endometriosis.
Missed or chronic infections
In some women, the immune system appears to remain in a prolonged state of activation, sometimes due to infections that are missed, under-treated, or lingering. This does not mean infections cause endometriosis, but they can add to inflammatory load and symptom burden in certain individuals.
Depending on history and symptoms, this may include viral reactivation patterns such as EBV, urogenital infections like Ureaplasma or Mycoplasma, gut infections including parasites, or recurrent bacterial or fungal infections.
Oxidative stress
Oxidative stress occurs when inflammatory and metabolic demand exceeds the body’s capacity to buffer and repair tissue. In endometriosis, oxidative stress can arise from immune activation, altered hormone signalling, impaired antioxidant capacity, and iron-related processes within the pelvic environment.
This can contribute to pain sensitivity, fatigue, and flare frequency.
Methylation and fertility outcomes
Methylation is a fundamental biochemical process involved in hormone metabolism, detoxification, inflammatory regulation, and antioxidant production.
In endometriosis, where oestrogen signalling, inflammation, and immune activity intersect, methylation efficiency can influence hormone clearance, inflammatory tone, and tissue resilience. In some cases, it may also be relevant to fertility outcomes.
Neuro-angiogenesis and why pain can linger
Endometriosis tissue can develop its own blood supply and nerve supply. This process can make pain feel intense and persistent, and it helps explain why pain may continue even when lesions are removed or appear inactive. The nervous system itself can remain sensitised.
Chronic stress, nervous system overload, and boundaries
Chronic stress influences pain, inflammation, hormones, and immune function. Many women with endometriosis have spent years pushing through symptoms, over-functioning, or carrying a disproportionate load.
Common patterns include difficulty resting, saying yes when capacity is already stretched, or feeling unable to slow down without guilt. These are understandable adaptations to chronic pain, but over time they can keep the nervous system switched on and make recovery harder.
Coagulation issues
Coagulation refers to how the body forms and breaks down blood clots. Some women with endometriosis experience bleeding and clotting patterns such as heavy bleeding, clots, or prolonged periods, which can contribute to iron depletion and inflammatory load. This is taken into account when assessing iron status and symptom patterns.
Environmental exposures and endometriosis
Environmental factors can add extra load to hormone processing, immune regulation, and inflammation. Examples include mould and mycotoxins, chemical exposures from plastics, pesticides, and solvents, and cumulative low-level exposures over time. In sensitive individuals, these may also worsen histamine-related symptoms.
Not all of these drivers apply to everyone. The aim is to identify which ones matter most for you.
Understanding Overlapping Conditions with Endometriosis for Holistic Care
Endometriosis frequently overlaps with other conditions, reflecting shared drivers such as inflammation, immune activation, hormone shifts, and nervous system sensitisation.
These may include adenomyosis, IBS-type gut issues, coeliac disease, thyroid conditions, bladder pain syndrome, pelvic floor dysfunction, migraines, fibromyalgia-type pain, chronic fatigue or post-viral patterns, hypermobility traits, histamine intolerance, and mood changes related to chronic pain and poor sleep.
Why this whole-body context matters
Endometriosis symptoms are rarely driven by a single factor. Pain, inflammation, hormone sensitivity, immune activity, and nervous system load often interact and shift over time.
Understanding your individual pattern helps explain why symptoms fluctuate, why some approaches help temporarily, and why decisions about surgery, medication, fertility support, or long-term management are rarely straightforward. This context allows care to be proactive and informed, rather than reactive when symptoms escalate.
Frequently Asked Questions About Endometriosis
Find answers to common questions about endometriosis, naturopathic care, and Alexandra’s services.
Yes. Many women have both, and overlap can affect symptoms and treatment decisions.
It can for some women. Research suggests around 30–50% of women with endometriosis experience fertility challenges, although many still conceive naturally.
There isn’t one best approach for everyone. Support is most effective when personalised and integrated with medical care.
For many women, yes, particularly when changes are targeted and realistic rather than restrictive.
'For many women, a diagnosis answers what is happening, but not why...'

Conquer Endometriosis Naturally Program
If you’re feeling lost and overwhelmed trying to figure out the best way to reduce your Endometriosis symptoms then follow this link to find out more about my Conquer Endo Naturally Program
If you’re looking for endometriosis naturopathic support that takes a whole-body, evidence-aware approach, follow the link below to learn more then book a consultation or discovery call.
Telehealth Care
Convenient Online Consultations
I specialise in helping women. Endometriosis diagnosis, reproductive challenges & disease, hormone imbalances & all other female related conditions.
Seeing me is easy. I offer appointments via Zoom, Facetime or on the phone.If symptoms are affecting your quality of life, accessing care should feel simple.
Through telehealth, I provide expert naturopathic support for endometriosis, hormone imbalance, fertility and broader women’s health concerns, available across Australia, New Zealand and the US. Personalised care from the comfort of home.

Related Resources:
Endometriosis and Sleep Disorders
Women with endometriosis often face more frequent complaints of poor sleep, reduced quality of life, and
The Importance of an Endometriosis Ultrasound
If you have endometriosis and/or you are looking for an endometriosis diagnosis, it is imperative
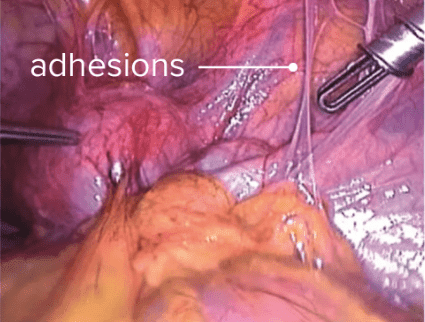
How to Break Down Endometriosis Adhesions
Endometriosis adhesions are a common but often misunderstood complication of endometriosis. These adhesions, or bands
EXCELLENTTrustindex verifies that the original source of the review is Google. I love that I can have each appointment via Zoom. Perfect for my busy schedule. And Alex is wonderful and so knowledgeable. My health has benefitted greatly is so many areas since joining her program in April. Very grateful and thankful.Posted onTrustindex verifies that the original source of the review is Google. I started seeing Alex back in January, and since then my health has improved so much. My endo symptoms are gone. I have energy again! I rarely get sick anymore, my immunity has improved so much. My sinus symptoms have improved. Overall I feel more calm and in control of my health again. Alex is very knowledgeable and empathetic, and I'm so grateful for the guidance she's given me. Thank you again Alex for everythingPosted onTrustindex verifies that the original source of the review is Google. After long time of feeling stuck with endo and fatigue, I started working with Alexandra which is when things began moving in a positive direction for me. Working with her for almost a year has been life-changing. My period pain level already decreased from 7-9 to 2-4 and we expect further improvements. Another win is that I am now getting off of antidepressants which is highly supported by the improvement of my overall health, as well as finding support and agency in alleviating my long-lasting symptoms. Alex always impresses me with the depth and complexity of her knowledge and research. At the same time she is attuned to and accepting of my rhythm and current capacity, making this big undertaking of healing endo at its roots, a stress and pressure-free experience. Alex is an exceptional practitioner, and I believe that our work together will benefit me for years to come.Posted onTrustindex verifies that the original source of the review is Google. I can't express enough how grateful I am for Alex's guidance and care. I started seeing Alex in 2023 when I was struggling with multiple health issues, and she has been an unwavering source of support and knowledge ever since. She's taught me so much along the way & has changed my life for the better. Thanks to Alex I've been able to manage stage 4 endometriosis without needing any further surgeries since being under her guidance, and my periods are now pain-free. She's also been instrumental in helping me with histamine issues and mold exposure. Beyond her expertise she is so kind + caring and has always made me feel heard since day one. I highly recommend Alex!!! She's made a world of difference in my health + getting my life back and I'm forever thankful to have had her on my side through it all.Posted onTrustindex verifies that the original source of the review is Google. I have been seeing Alex since November last year after a severe endometriosis diagnosis post laparoscopy. I was so overwhelmed about moving forward with this illness until I found Alex. She understood my situation completely and I felt supported and heard from our first consultation. I improved from the first month of treatment, and now, only 4 months in, I feel like a completely different person. I am back living a full life and my pain symptoms are already more than halved, something I personally haven't been able to achieve with other treatment options. Her treatment plans are detailed and extremely knowledgeable, incorporating the latest scientific research and natural medicine practices, and we have slowly introduced lifestyle and diet changes and supplements over time, making things extremely manageable. I truly can't recommend Alex enough!Posted onTrustindex verifies that the original source of the review is Google. I started seeing Alex in April 2023 for management of my severe endometriosis and adenomyosis following a laparoscopy. I discovered Alex through listening to a podcast on endo and was impressed with her extensive knowledge and holistic approach to managing endo. Through working with Alex and following her advice, my pain has significantly reduced and my quality of life has dramatically improved. Alex also supported me to fall pregnant, give birth and navigate postpartum. Cannot recommend Alex enough - she is incredibly knowledgeable, supportive, empathetic, caring, understanding and responsive!Posted onTrustindex verifies that the original source of the review is Google. We have seen multiple naturopaths and integrative GPs. Alex has been the only practitioner with a focused and results oriented approach. My daughter went from monthly agony to no pain in 3 months. We are beyond grateful for Alex’s knowledge and expertise. It’s literally been a total game changer.Posted onTrustindex verifies that the original source of the review is Google. Alex is the real deal! She is just as committed to my health as I am, if not more. It's evident in every interaction how committed Alex is to her craft. She's up to date with latest research and lives and breathes what she preaches. I started seeing Alex following surgery to remove severe endometriosis and I feel so at ease with her in my corner. We're getting to the root cause of issues and reviewing habits I had no idea were even linked to endo! I'm finally learning how to care for my body :)Posted onTrustindex verifies that the original source of the review is Google. I’ve been seeing Alex for over a year now. I came to Alex for help with fertility and endometriosis/adenomyosis management. Alex has been a huge support through my fertility journey, with rigorous testing and supported diet/supplements that have helped me to fall pregnant this year. Alex has a holistic approach to health and is very knowledgeable - thanks for everything Alex.Posted onTrustindex verifies that the original source of the review is Google. I was in such a desperate state before I found Alex. I'm doing so so much better since I've learnt about histamine and mould. Completely life transforming, I feel like I've got my life back again. Thank you so much for your help. I've been telling everyone that will listen about you.
Short medical disclaimer: This information is general and educational and is not a substitute for medical advice, diagnosis, or treatment. Please work with your healthcare team for individual care.